Since becoming popular in the 1950s, the Bricker ileal conduit continues to be the most frequently utilized urinary diversion technique following radical cystectomy.1 The conduit typically involves using a 15 cm-20 cm segment of the terminal ileum harvested at least 15 cm proximal to the ileocecal valve.1 Patients generally report high quality of life after the procedure,2 despite being incontinent and relying on an external appliance for urine storage. However, various complications, and fear of complications, can decrease the quality of life in patients with ileal conduits.2
While common, reported rates of stomal complications vary widely, occurring in 15%-65% of ileal conduit cases, the majority of such events occur at the level of the skin and are affected by the choice of ileostomy technique.3 Stomal stenosis, parastomal hernia, and skin irritation are common complications, affecting up to 15%-20% of patients.4,5 These complications have been well studied in the literature, while complications including stomal prolapse and retraction have been studied less. Yet, when they occur, they can decrease a patient’s quality of life after an ileal conduit procedure.
Traditional teaching on stoma formation has focused on the end ileostomy, often termed the “rosebud” or nipple stoma, or, in obese patients, the loop end ileostomy or “Turnbull.” The “rosebud” is generally formed by pulling a 5 cm-6 cm portion of ileum through the abdominal wall, intussuscepting it, and suturing it down to the skin.6 In obese patients, who often have short mesentery to complement their thick abdominal wall, the Turnbull offers an acceptable alternative. That said, the senior author has had good results using the herein described technique in obese patients without stomal retraction, a flush stoma or the need to use the Turnbull technique.
Given the high rate of stomal complications, multiple groups have reported on techniques to decrease or eliminate stoma related complications.7 At our institution, we have modified the traditional technique with the use of large, blunt, right-angle forceps which facilitate intussusception and maturation of a rosebud stoma. Herein we describe our technique, which aims to prevent the creation of a shallow stoma and the resulting sequelae.
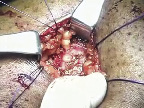
After the ureteroileal conduit anastomoses have been completed (utilizing a shield-shaped conduit serotomy8) and single J ureteral stents (positioned through the conduit using a rigid, clear Yankauer suction tip) secured to distal conduit mucosa (2 cm from the end of the conduit) with 4-0 Chromic suture, the stoma site is made by creating a 2 cm diameter circular anterior rectus fascia defect using electrocautery. Through the edge of the anterior rectus fascia circular defect, 2-0 Vicryl sutures are placed at the 12, 3, 6, and 9 o’clock positions, Figure 1.
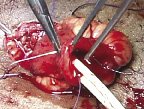
Once these sutures are placed, a Kelly clamp is used to spread through the rectus muscle, creating the opening through which the stoma will pass. The index and middle fingers are then passed through the opening to confirm that it is of adequate size. Next, a Babcock clamp is used to bring the distal end of the conduit and ureteral stents through the opening in the abdominal wall. The conduit is pulled gently until resistance is met. The previously placed 2-0 Vicryl sutures are then passed through the serosa of the ilium at the level of the rectus fascia, parallel to the ileal blood supply, and tied down, Figure 2.
Next, four additional 2-0 Vicryl sutures are placed at the 12, 3, 6, and 9 o’clock positions through the skin edge. These sutures are then placed in the ileal serosa at or just below skin level, parallel to the blood supply, followed by a continuation of the stitch placement through the distal end of the ileal conduit, with the 12 o’clock and 3 o’clock sutures placed immediately adjacent to the ileal mesentery. The 6 o’clock and 9 o’clock sutures are spaced evenly between.
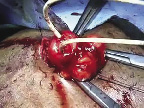
Once the four additional sutures have been placed, large, blunt right-angles are placed at the mid-aspect of the ileum protruding above the skin and used as a fulcrum to facilitate intussusception of the rosebud stoma. Multiple right-angles can be utilized at this point of the procedure to help facilitate circumferential intussusception of the stoma, Figure 3.
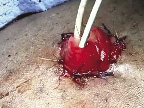
After intussusception is completed, the four previously placed sutures are tied down to secure the rosebud stoma in position. Two or three interrupted 4-0 chromic sutures are placed between the 2-0 Vicryl sutures. A catheter is not placed as in our experience the single J ureteral stents are sufficient to ensure renal and conduit drainage, Figure 4. With the rosebud stoma completed, a pelvic drain is placed and the operation completed.
The use of multiple blunt right-angles aids in the eversion or intussusception of the rosebud stoma around the entire circumference of the newly created stoma. By using the right-angles as a fulcrum, gentle eversion is easily accomplished. Moreover, this technique prevents the creation of shallow stomas or stomas that are not adequately circumferentially everted. We consistently create stomas that are 2 cm to 3 cm in height and, in our experience, have not had significant problems with skin or stoma irritation, stomal stenosis orstomal retraction. Additionally, by placing two sets of 2-0 Vicryl sutures, we have not seen problems with ileal prolapse. The senior author has found this technique effective in the obese, creating a 3 cm diameter circular anterior rectus fascial defect, dilated with usually two or occasionally three fingers when necessary to allow adequate ileal mobilization through the abdominal wall.
Stomal complications are very common, occurring in up to 65% of ileal conduit cases.3 Stomal stenosis and parastomal hernias are two well-studied complications that are fairly common following ileal conduit procedures. Stomal stenosis rates have been reported in 2%-19% of cases4 and ischemia is thought to be the underlying cause but a flush stoma, allowing the skin to constrict, is a likely contributing factor. This complication is more common in patients with an end ileostomy.8 Parastomal hernia is another common complication with rates ranging from 10%-15% in patients receiving an ileal conduit following cystectomy.4 Overweight and obese patients are at increased risk for parastomal hernias, as are patients who undergo a Turnbull ileostomy9 or those who have the stoma placed lateral to the rectus abdominis, instead of directly through it. Skin irritation is another relatively common complication with an incidence of 14%-20%.5 Shallow stomas or stomas placed in improper locations are a common cause of such irritation. In such cases, urine can leak onto the skin causing irritation and dermatitis and is often the result of an improperly fitting stomal appliance. Such irritation can lead to stomal stenosis and even submucosal lymphoid depletion or fibrosis.10
There are a number of additional, less common complications seen following conduit formation. Stomal prolapse is a rare complication with an incidence rate of 1.5%-8%.5 Prolapse can be managed with a prolapse belt, in a non-surgical fashion, but necrosis of the stoma can occur as a result. There is little research regarding stomal retraction, though one review estimated the complication occurred in 9%-15% of ileal conduit procedures.5 The underlying cause is thought to be a result of tension on the stoma from inadequate bowel mobilization or a thick abdominal wall.
Since adopting the use of blunt right-angles in facilitating the intussusception of the rosebud stoma, we consistently create stomas that are 2 cm-3 cm in height above the abdominal wall. Our results utilizing the blunt right-angles have been very positive. The protruding everted end of the ileal conduit, facilitates proper fitting of the appliance, working to prevent skin irritation and the resulting sequelae. Additionally, it works to prevent skin edge constriction seen with flush or retracted stoma stenosis.
Further study is needed to determine the absolute rates of postoperative stoma related complications, although the senior author has observed no cases of stomal stenosis, retraction or prolapse in approximately 60 sequential cases using this technique. To our knowledge this is the first description of a surgical technique that aims to maximize the length of the rosebud portion of the ileal conduit so as to improve ease of use and minimize conduit related complications.
The use of right-angles to aid in intussusception when creating a Bricker ileal conduit is simple, easily implemented and effective. It provides consistent results that produce an aesthetically pleasing stoma and works to help reduce many common complications associated with ileal conduits.

 Indexed in Index Medicus and Medline
Indexed in Index Medicus and Medline